The Evolution Of Breast Density Scales & Automated Algorithms
Nov 29, 2019Categories: Blog, Breast Cancer Risk, Breast Density
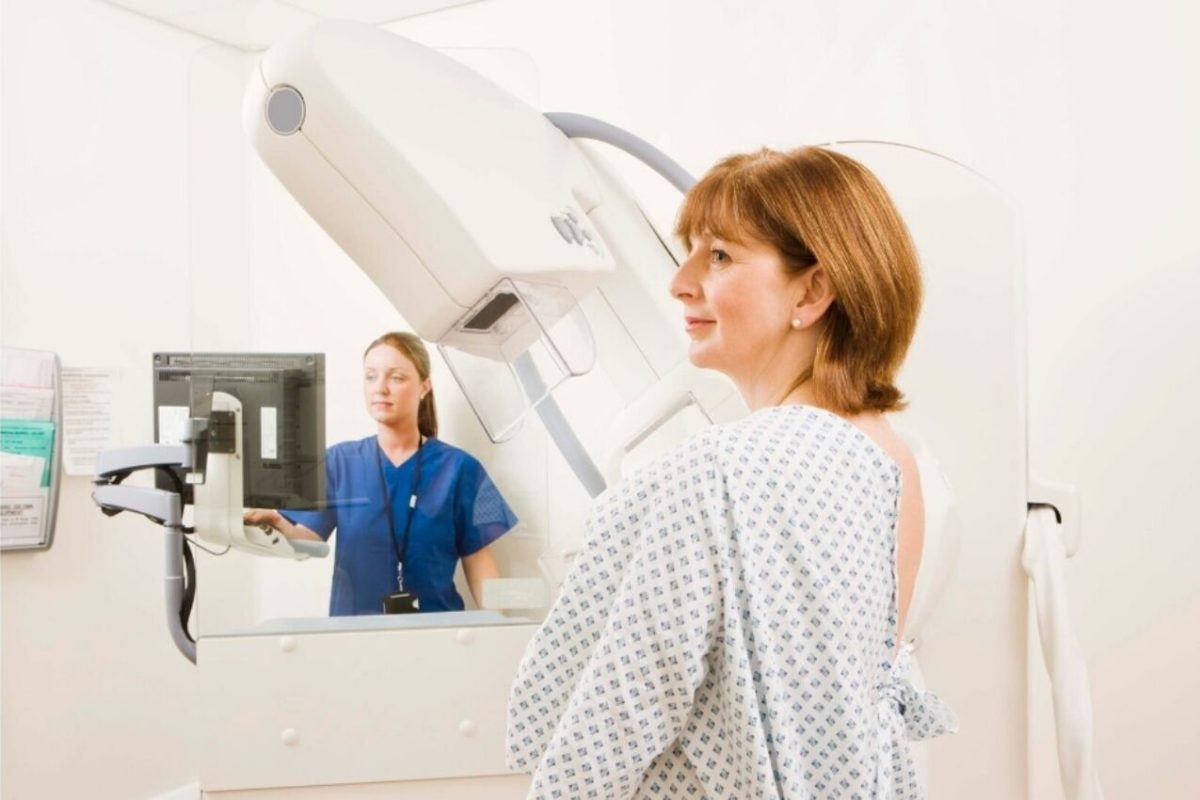
Breast density is an established independent risk factor for breast cancer. Women with extremely dense breasts have a 4-6x increased risk of developing breast cancer compared to women with fatty breasts. Research shows that risk models that incorporate breast density predict breast cancer better than those that do not.

The FDA recently recognized the important relationship between breast density and breast cancer risk in policy changes to modernize its oversight of mammography services.
On a mammogram, dense breast tissue is visually similar to cancer (both appearing white) meaning that dense tissue can mask the presence of cancer.
It is widely acknowledged that mammography is the best available frontline tool for early cancer detection. But given the decreased sensitivity due to the masking effect of breast density, mammography alone as a screening strategy is not appropriate for every woman. Mammography misses roughly 50% of cancers in very dense breasts.
Mammography plays an important role in risk-based and individualized population-wide breast cancer screening strategies designed for early breast cancer detection. But due to the increased risk of missed cancers in dense breasts, a radiologist may recommend supplemental imaging with a more sensitive screening modality for women with dense breasts.
The visual assessment of breast density – the current standard of care – is highly variable.

A woman may be told she has dense breasts by one radiologist and fatty by a second. This subjectivity is most evident in cases for which density falls just on either side of the 50% breast density threshold per the ACR BI-RADS® Atlas 4th ed. breast density grade.
To address this issue, the ACR BI-RADS® Atlas 5th ed. re-defined breast density grades using a categorical scale to describe breast density qualitatively. The new scale emphasizes the masking effect of mammographic density.
The variability in the visual assessment of breast density has important consequences for clinical decision-making and healthcare resource allocation, as the density result can affect follow-up care. A woman whose mammogram is assessed by one radiologist to be ‘not dense’ may not receive a recommendation for follow-up with a more sensitive screening modality, while a second radiologist may determine that the mammogram has dense breast tissue and direct her to adjunctive screening such as Ultrasound or MRI.

Standardization of breast cancer screening follow-up protocols requires individualized risk-based screening to be applied at a population and health system level in a way that enables appropriate service delivery and effective resource management.
That’s where automated breast density solutions come in. The reproducible assessments generated from algorithms facilitate standardized recommendations upon which tailored risk-based care depends.
Mammographic Density is All About the Pixels
The rendering of breast density on a mammogram in a clinical setting is referred to as mammographic density and is what the radiologist sees and evaluates when reviewing a mammographic exam.
In clinical practice, the radiologist evaluates a 2-D image that appears in varying levels of brightness, textures and patterns. So pixel intensity, pattern and texture define the appearance of breast density on a mammogram.
The ACR BI-RADS® Atlas specifically refers to assessing 2-D mammograms by evaluating the appearance of breast tissue composition as rendered on the mammogram.
Qualitative Breast Density Assessment
ACR BI-RADS® Atlas 5th ed.
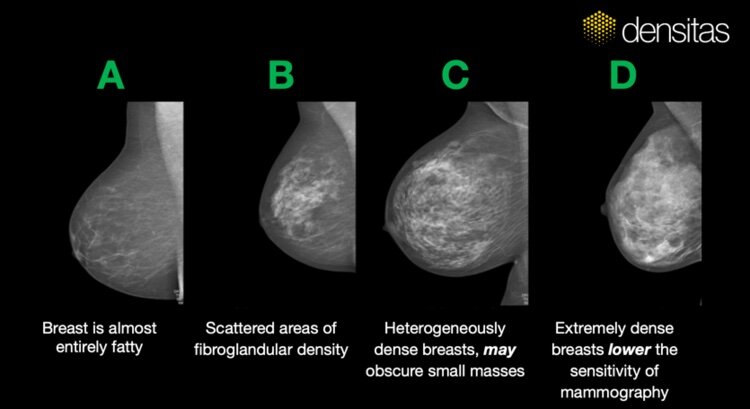
According to the American College of Radiology’s latest guidance on breast density classification, the ACR BI-RADS® Atlas 5th ed. guidance on qualitative classification of the appearance of breast composition, radiologists should factor in the appearance of breast density–its texture and distribution–when evaluating a mammogram for breast density to effectively set follow-up screening protocols that may direct the woman to MRI or Ultrasound, or may determine frequency of follow-up screening exam visits.
Quantitative Breast Density Assessment
ACR BI-RADS® Atlas 4th ed.
Quantitative assessment does not account for clusters of mammographic density. Percent density assessment reduces to a counting exercise whereby the radiologist simply visually assesses the amount of density perceived in the mammogram relative to total breast area.

A woman may be judged ‘not dense’ under the ACR BI-RADS® Atlas 4th ed. guidance on quantitative classification of the appearance of breast composition because her percent density falls under the 50% dense threshold. But that conclusion may not adequately account for the stronger masking effect that moderate concentrations of mammographic density may pose in an exam where the breasts otherwise present as ‘fatty’.
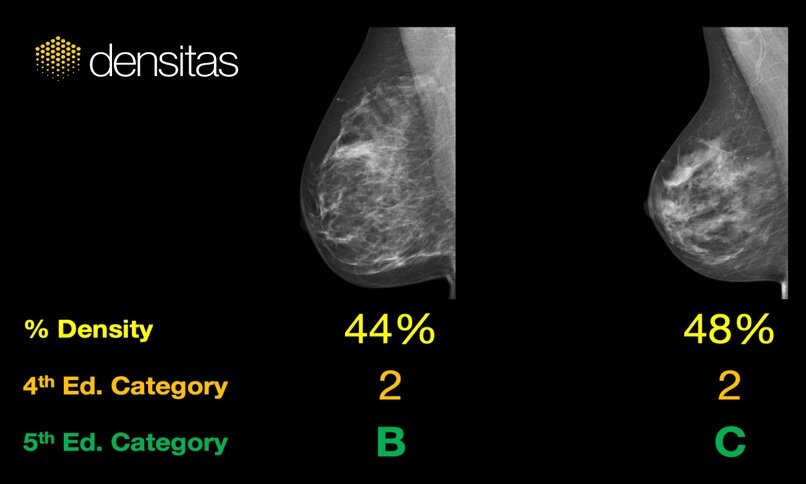
A radiologist following the modern ACR BI-RADS® Atlas 5th ed. guidance on qualitative classification, which recognizes the importance of density texture and distribution, may shift the same woman into the ‘dense’ category due to the appearance of clusters of breast density in the exam and their risk of masking cancer, affecting follow-up care as a result.
A Brief History of Breast Density Algorithms
Area-based Algorithms
These earliest algorithms are based on thresholding and segmentation of the pixels in the image to generate area-based percent mammographic density measurements. The early algorithms were operator dependent and semi-automated. Density measures are quantitative and in that sense aligned with the ACR BI-RADS® Atlas 4th ed. density scale.

Fig. 1 from Nickson, C., Arzhaeva, Y., Aitken, Z. et al. AutoDensity: an automated method to measure mammographic breast density that predicts breast cancer risk and screening outcomes. Breast Cancer Res 15, R80 (2013) doi:10.1186/bcr3474. Copyright © 2013, Springer Nature.
These algorithms processed digitized, and then later digital, clinical use mammograms, and have been typically used for research purposes. Percent density values typically range from 0 – 100% that are thresholded to derive categories aligned with the ACR BI-RADS® Atlas 4th ed. density scale.
Volume-based Algorithms
The next stage in the evolution of breast density algorithms was driven by the goal to estimate percent dense breast tissue volume based on absolute and relative physics models. These physics models depend on assumptions relating to a number of physics acquisition parameters, including breast thickness, and on the ability to precisely identify a ‘fatty’ reference set of pixels. Percent density measures are quantitative and aligned with ACR BI-RADS® Atlas 4th ed. (2003) density scale.

Raw ‘for processing’ (top row) vs clinical ‘for presentation’(bottom row) images. Fig. 1 from Burton, A., Byrnes, G., Stone, J. et al. Breast Cancer Res (2016) 18: 130. https://doi.org/10.1186/s13058-016-0787-0 is licensed under CC BY 4.0
With the introduction of the ACR BI-RADS® Atlas 5th ed. (2013) density scale that moved away from the previous quantitative density scale, these volumetric density scales remained fundamentally unchanged and at their core quantitative. These algorithms can only process raw ‘for processing’ images. Percent density values typically range from 0 – 45% and are thresholded to derive categories aligned with both the ACR BI-RADS® Atlas 4th ed. and 5th ed. density scales.
Machine Learning Algorithms
A major move forward from volumetric algorithms was the emergence of machine learning algorithms that were based on hand-crafted image features derived from pixel patterns, textures intensities, histogram features and other physics acquisition parameters.
These algorithms were the first to leverage statistical and machine learning methods and train on large labelled sets of mammograms. In so doing, these algorithms could be either developed to generate a quantitative percent density measure, or to generate a qualitative classification of density. These algorithms can be trained to process either raw or clinical use mammograms.
Deep Learning Algorithms
Deep learning represents yet another significant leap forward in the evolution of breast density algorithm development that especially aligns with how the visual cortex processes images.

Projection of breast tissue onto a mammographic image is manifested as mammographic density to the retina and visual cortex.
Adapted from Kubilius, Jonas (2013): Ventral visual stream. figshare. Figure.
Deep learning algorithms have all the benefits of machine learning algorithms, with the added bonus that they discover the image features of importance without requiring them to be hand-crafted. They are self-learning. They generate breast density percent measures and density grades by analyzing the distribution, texture and intensity of the pixels in the images from either raw or clinical use images.
Similarly to machine learning algorithms, deep learning algorithms can be developed to generate both a quantitative percent density measure or a qualitative classification of density, and so align with both the quantitative ACR BI-RADS® Atlas 4th ed. (2003) density scale, and with the qualitative ACR BI-RADS® Atlas 5th ed. (2013) density scale.
The Future Is Now

Breast density algorithms have evolved significantly over the past 25 years to align better with how a radiologist actually visualizes breast density in a mammogram. Modern A.I. solutions are essential to generate density reports that align with density reporting guidelines.
The challenges regarding use of raw images is that they are rarely archived in PACS and are unavailable for retrospective processing. Additionally there is poor face-validity between what a radiologist sees in a standard ‘for presentation’ clinical use mammogram and what appears in a raw ‘for processing’ mammogram.

Practically and pragmatically, clinical ‘for presentation’ images have excellent face-validity with what the radiologist is seeing, and are ideally suited for simplified deployment in clinics and deep integration into reporting and PACS workflows, making clinical adoption much easier.
Discover what a PACS-centric, A.I.-powered automated breast density solution, that research shows is strongly associated with cancer risk and represents a practical method for breast cancer risk assessment, can do for your imaging center or health system.
Let’s Stay Connected, Subscribe for Updates
Join our email list to stay up to date on the latest advancements in breast health technology.
 Canada
Canada USA
USA UK
UK